As a healthcare professional there is a skin condition that you will occasionally be presented by patients usually after exposure to some medications. It is a worrying presentation no matter how many years of practice you may have. I took a lot of information on Stevens-Johnson syndrome/toxic epidermal necrolysis from the National Institute of Health (NIH), August 2018.
Stevens-Johnson syndrome/toxic epidermal necrolysis (SJS/TEN) is a very severe reaction, most commonly triggered by medications, that causes skin tissue to die (necrosis) and detach. The mucous membranes of the eyes, mouth, and/or genitals are also commonly affected.
SJS and TEN previously were thought to be separate conditions, but they are now considered part of a disease spectrum. SJS is at the less severe end of the spectrum, and TEN is at the more severe end. It is considered SJS when skin detachment involves less than 10% of the body surface. It is considered toxic epidermal necrolysis (TEN) when skin detachment involves more than 30% of the body surface. People with skin detachment involving 10-30% of the body surface are said to have “SJS/TEN overlap.” All forms of SJS/TEN are a medical emergencies that can be life-threatening.
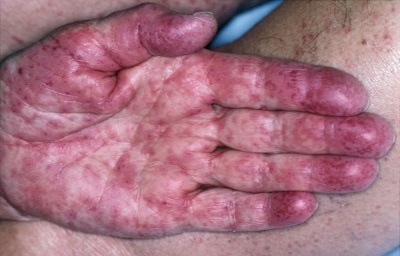
The first symptoms of SJS/TEN often include fever and flu-like symptoms (such as general ill feeling, body aches, and cough). Within about 1 to 3 days, a red or purplish rash forms, and then the skin begins to blister and peel, leading to “raw” areas of skin that are painful. This often starts on the face and then spreads to other parts of the body. These skin symptoms usually begin on the face and chest, and then spread to other parts of the body. The mucous membranes may also become involved during this time, which can lead to symptoms such as severe conjunctivitis (when the eyes are affected), trouble swallowing and breathing (when the mouth and airway are affected), and difficulty urinating and genital pain (when the genitals are affected).
The mucous membranes (thin, moist tissues that line body cavities) of the mouth, throat, genitals, eyes, and/or digestive tract usually also are involved, and may become affected before or after the skin. Early symptoms of mucous membrane involvement may include light sensitivity, itching or burning of the eyes, and pain when swallowing. As the condition progresses, eye symptoms may include pain, severe conjunctivitis, discharge, iritis, and corneal blisters.
Eye involvement can lead to long-term eye complications, including vision loss. Symptoms of mouth and throat involvement may include painful blisters, and trouble swallowing and breathing. Symptoms of genital involvement may include inflammation of the urethra, vaginitis, painful blisters, and difficulty urinating. Gastrointestinal symptoms may include diarrhea, black or tarry stools.
Symptoms may persist or worsen for up to two weeks before the skin and mucous membranes begin to start healing themselves. Skin that remained attached may gradually peel during this time, and the nails may shed in some cases.
SJS/TEN often is triggered by certain medications including allopurinol, anti-epileptics, pain relievers (e.g.NSAIDS), cancer therapies, or antibiotics (sometimes up to 2 weeks after stopping the medication).Antibiotics are the most common cause of Stevens-Johnson syndrome, followed by analgesics, cough and cold medication, NSAIDs, psycho-epileptics, and antigout drugs. Penicillins and sulfa drugs are the most antibiotics associated with SJS/TEN. Ciprofloxacin has also been linked to the condition.Most anticonvulsant-induced SJS occurs in the first 60 days of use. Some antiretroviral drugs have been implicated in SJS (Medscape, January 2019).
SJS/TEN can also be triggered by infections such as pneumonia, herpes virus, and hepatitis A. In many cases the cause cannot be identified. People that may be at increased risk to develop SJS/TEN include those with HIV, a weakened immune system, a personal or family history of the condition, and certain variations of a gene called HLA-B. The incidence of the condition among people with HIV is about 100 times greater than among people in the general population.
There are no universal diagnostic criteria for SJS/TEN. Currently the diagnosis is based on the person’s medical history and symptoms. People suspected of having SJS/TEN should be admitted to the hospital to confirm the diagnosis and assess severity. Whether a person is diagnosed specifically with SJS, TEN, or SJS/TEN overlap depends on the percentage of body surface area affected.
Treatment needs should be assessed in the hospital to determine severity and where treatment should be provided (e.g. intensive care unit, burn unit, or dermatology unit).Generally, treatment of skin symptoms is similar to that of major burns, and includes wound care, pain control, fluids and electrolytes, nutritional support, temperature management, and monitoring for or treating secondary infections.
Treatment may involve stopping a triggering medication (for those suspected of having medication-induced SJS/TEN), standard therapies used for major burns, various eye treatments (for those with eye involvement), pain control, and preventing and treating infections.
The overall mortality rate for SJS/TEN is about 25%, ranging from about 10% for SJS to over 30% for TEN. The most common causes of death include sepsis, acute respiratory distress syndrome and multiple organ failure. Those that survive may experience recurrence (particularly if re-exposed to a trigger) and/or long-term complications involving the skin and affected mucous membranes.
The long-term outlook and chance of recovery varies from person to person. Regrowth of the affected skin typically occurs in two to three weeks, but recovery can take weeks to months, depending on the severity of symptoms. Feelings of overwhelming tiredness may persist for months. Depression may also develop. For some, complications may develop within weeks to months of an acute episode, and there may be long-term complications involving the skin and affected mucous membranes, which can severely impact quality of life.
As a pharmacist always get your pharmacovigilance forms ready to assist the healthcare team to identify possible the offending agent.
DR. EDWARD O. AMPORFUL
CHIEF PHARMACIST
COCOA CLINIC



